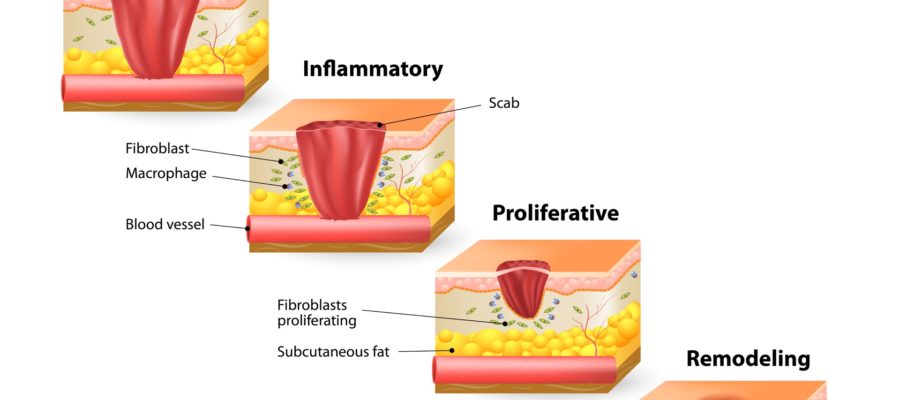
The term chronic wounds includes those wounds that do not heal naturally and requires an appropriate specialist care. Chronic wounds can be divided into:
- Post-traumatic This category of injury is secondary to a traumatic event that damages skin and underlying soft tissues, compromising local vascularization. Fractures and muscle injuries could be associated. The damage to soft tissue is too often underestimated and requires a specialistic evaluation
- Surgical wounds. Rarely surgical wounds could have a healing delay and become chronic. Wound dehiscence is therefore observed, sometimes along with skin necrosis in the surrounding region. The causes are several and should be always investigated. Systemic causes could be diabetes, vascular diseases and Local factors include excessive tension of wound margins, inadequate suture or wound infection. Wound dehiscence could compromise surgery (e.g. leading to exposure of bone and internal fixation or exposing an abdominal patch).
- Vascular ulcers.They are often produced by a lack of blood supply. Generally they occur at the extremities (especially the lower limb) and can be classified in arterial, venous or mixed depending on the primary etiologic factor (respectively a problem in arteries, veins, or both).
Wound management
Treatment and management of chronic wounds is specialistic task and should be customized on each patient. A multi-specialist approach is often necessary; the Plastic Surgeon has a key role in the treatment of soft tissues and should coordinate management of chronic wounds and reconstruction. The therapeutic strategy may employ one or more of the following therapeutic and surgical devices:
- Advanced wound dressings
- Dermal and skin substitutes
- Skin grafts
- Autologous keratinocytes
- VAC therapy (Vacuum Assisted Closure)
- Flaps
Advanced wound dressings
These dressings are able to stimulate and accelerate healing. This broad category of dressings includes hydrogels, alginates, collagenase and many others. These dressings should be prescribed by a specialist according to the type of wound and its evolution.
Dermal and skin substitutes
These consist of matrices of hyaluronic acid or collagen (human or animal) that are positioned with a surgical procedure over wound. These substitutes are then inhabited by the cells of the host, thus regenerating a layer of tissue. To accelerate healing, it is possible to perform a second procedure of skin grafting, in order to restore a complete cutaneous layer. The quality of reconstruction with substitutes is inferior compared to cutaneous expansion, however it allows the reconstruction of large areas.
Skin grafts
A skin graft is a thin layer of skin that is harvested with a short surgical procedure and applied to the wound. The graft is able to survive creating new vascular connections and to restore a cutaneous layer. They could be classified according their thickness in thin (0.25mm), medium-thickness (0.7 mm) and. full thickness grafts (when they include the whole cutaneous layer). Skin grafts usually require one week to take in the new site. During this time a compressive dressing is employed to allow a proper healing. In case of thin or medium size grafts, the color of the donor skin keeps a different pigmentation than the surrounding skin. Full thickness skin grafts instead are excised with a linear scar.
Engineered tissue - autologous keratinocytes
This advances reconstructive solution is produced by in vitro cultivation of autologous keratinocytes (harvested from patient with a little procedure). Once the desired number of cells is harvested, these are seeded on a inert sheet and applied on the wound with a short surgical procedure. This solution allows the reconstruction of large wounds with a minimal quantity of cells. This option is therefore an alternative to skin grafts, when a donor site is not available (or not sufficient) or the patient prefers to avoid any scar at the donor site.
The cost of this procedure is still elevated.
VAC therapy (Vacuum Assisted Closure )
This particular dressing is able to apply a negative pressure on a wound. The aim is to absorb wound secretion and to promote granulation tissue. This dressing has the following indications:
- Heavily secreting wound (without infection)
- Poor granulation
- Deep wounds in which a strong granulation is required
Flaps
Flaps allow to repair in one surgical procedure large defects with autologous tissue. This procedure should be indicated for deep, wide and complex wounds where the other solutions are not applicable or when an faster resolution is desired. Flaps could be classified in:
- Local flaps. These flaps are composed by skin and a small portion of subcutaneous tissue. Local flaps are supplied randomly by dermal vasculature and allow the reconstruction of small areas. The aesthetic outcome is good.
- Pedicled flaps. Pedicled flaps consist in a portion of tissue supplied by a pedicle (usually an artery and vein). A pedicled flap may include not only skin but also fascia and muscle. This solution allows to reconstruct medium size areas. The flap could reasonably reconstruct defects as far as the length of the pedicle.
- Free flaps. This solution allows the reconstruction of large and distant defects. They may include skin, muscle or bone segments. The pedicle of the flap is cut and re-connected (in jargon anastomosed) to the vessels of the acceptor site. Requires the use of a microscope to connect the vessels and a longer operative time.